I’ve done articles like this in the past, comparing my clinical results over the years.
But I’ve just hit what feels like another milestone, so I’m going to re-do it using my current reporting tools.
I’m going to show data from four points in time:
- 2017, when I’d only recently started using an Automated Insulin Delivery (AID) system.
- 2020, when I’d tuned the AID system in Hybrid Closed-Loop (HCL) mode pretty well.
- 2022, when I was still trying to get “Fully Closed-Loop” (FCL) mode working the way I wanted.
- 2023, when I may have got my head (and tools) around FCL mode.
You can of course skip ahead to the comparison, but hopefully it won’t take long to read through them in sequence.
Then there’s a bit of discussion and analysis. A reply to assumptions that I must be living a low-carb lifestyle, and thoughts about the path from here.
Early Looping, 2017 |
(to start) |
This sample is from the second time I’d been back to my endocrinologist after starting to use a loop.
At the time I was using OpenAPS and a Medtronic Paradigm pump with Humalog. Some of this CGM data was from Libre1 sensors, but most was from Dexcom G5. The CGM was regularly calibrated from fingerpricks, so most of it should have been accurate.
This was a dramatic improvement over what I had been managing before looping! But what information can we take away from this table?
With 93.6% TIR (3.9-10) this was suddenly miles ahead of the classic “at least 70%” goal. In fact I was already getting 70.8% for what is now referred to as the TItR (3.9-7.8) range.
I was getting 1.3% TBR (<3.9). Again, this is a lot better than the classic goals. So I was hopefully being fairly safe regarding hypos. In fact more than half of that was just below 3.9 (it’s not unusual to see a gradual dip just below 3.9 and up again).
My glucose variability can be seen in the CV of 25%. Again that’s better than the 30+% often suggested as a starting point.
The CGM data predicted 6% (eHbA1c). And the blood taken on the 15th of November came back with an HbA1c of 5.8%. Not too far off!
With a CGM that gives data every 5 minutes, that makes a total of 288 possible datapoints per day. Of course, we have some gaps in this data. Things like sensor failures as well as 2-hour warmups all take away from the coverage. But in this data it captured around 97% of the possible points (an average of 281 out of 288) which isn’t terrible.
This is not the real-time data being used by the loop though: theoretically this could include back-filled data after outages (although at this time the apps I was using did not support that). But it’s still relevant that this is a fairly complete dataset.
Amulatory Glucose Profile (AGP)
Overlaying the data for all those 60 days shows the spread during the average day.
Again, not a result to be particularly unhappy about! While we’re sleeping is usually the easiest time for an AID system to cope, and the point in the graph where things jump up in the morning is obvious. But it wasn’t terrible!
I think it’s worth comparing with the data from a year prior when I had been using an Animas pump manually and using Libre sensors…
In comparison, the 2017 data was amazing!
What it was like
I was quite happy with these results. I felt happy I had taken positive steps for my health. But it didn’t feel like an end-point. I did have the “long game” in mind, in that I’d been prompted to set my loop up by the possibility for fully-closed operations with Fiasp (which had just been approved in Australia, although we didn’t get access to it for a few years). But even without those advanced features working for me yet, I felt comfortable I had a great system running.
I was interacting with the system a lot. I was counting carbs and bolusing for meals, and in fact doing various correction doses on top of that. A lot less “hand-holding” of the system than I used to have to do before the loop, but still I interacted with it fairly often.
Hybrid Closed-Loop, 2020 |
(to start) |
By now I was using AndroidAPS with a Combo pump, Fiasp insulin, and using Dexcom G5. So the kit of equipment I was carrying around was a lot more compact than it had been in 2017. I was still announcing my food and bolusing for meals, but the system was already managing a lot better control than I’d had when I started.
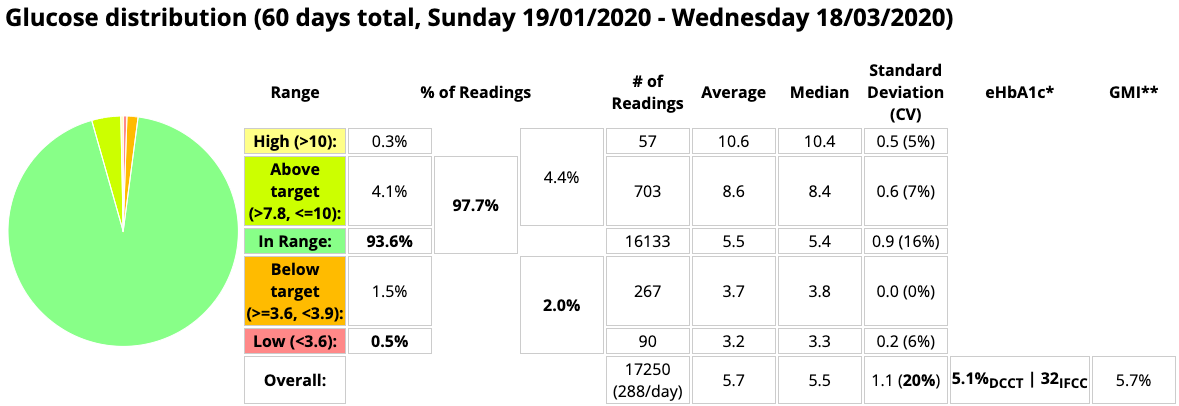
In short, I was very happy with these results!
TIR was 97.7%, and even TItR was 93.6%!
TBR had grown a little to 2%, but again most of that was just below 3.9 mmol/L. Still a long way below any “4%” suggestion.
CV (variability) had dropped to 20%. With some people without diabetes getting 17-18%, there didn’t seem a lot of room for improvement there.
The CGM data gave an eHbA1c of 5.1%, while the blood test the next day gave an HbA1c of 5.0%.
Interestingly, the CGM coverage was almost 100% (99.8%, but who’s counting?). By this time I was alternating transmitters and sensors to avoid the 2-hour warmup outages.
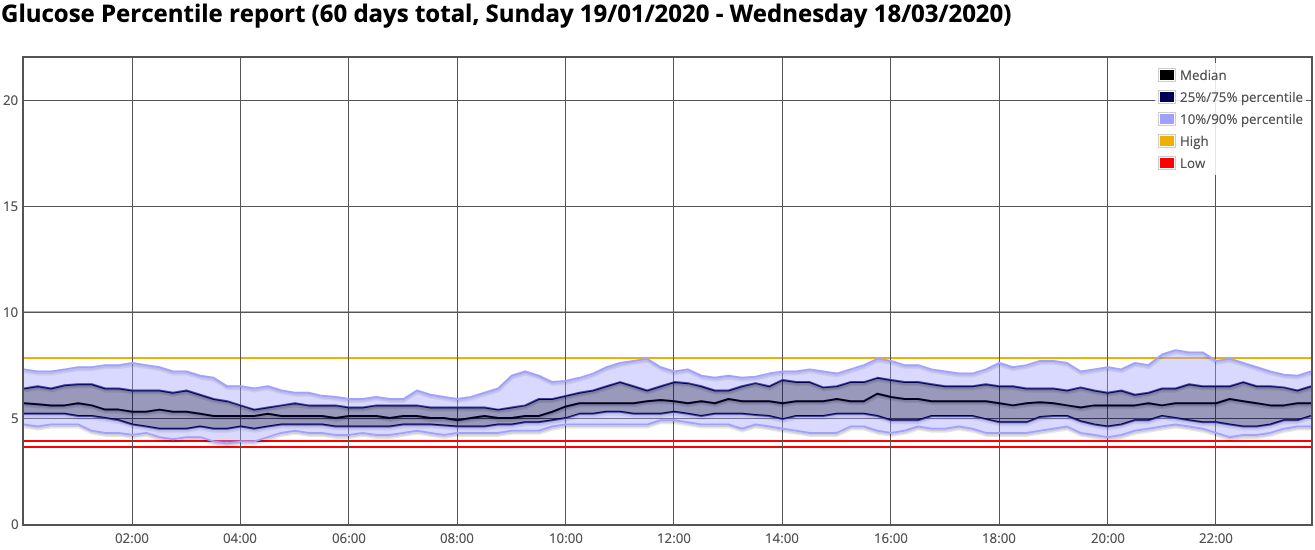
AGP
Looking at this it should be immediately obvious that I was getting a much tighter grouping than in 2017.
What it was like
Again, I was very happy with these results! An HbA1c of 5.0% (smack bang in the middle of the 4.4-5.6% reference range for someone without diabetes) was a new record for me.
Fiasp had definitely let the AID system improve performance. And I had tuned the system a lot better to suit me too.
However I was still counting all my carbs, and in fact declaring both carb and protein intake to the system. I was doing it in more detail than I had been in 2017. I was using less corrections than I used to though. Of course I also used temporary targets to announce exercise to the system.
I was paying a lot of attention to those things. I was getting great results, but in retrospect I was working fairly hard to achieve them.
Fully-Closed Loop, 2022 |
(to start) |
Two years on, I hadn’t counted/declared food or given any bolus for a year already.
I was still advising the system (with temporary targets) when I was going to be exercising though. So although the lack of inputs regarding food makes it feel like a fairly “fully-closed” loop, life isn’t completely “announce-less”.
I was still using AndroidAPS, mainly with Fiasp but starting to experiment with Lyumjev. My CGM was Dexcom G6. I don’t calibrate it to fingerpricks as often as I did with G5, but I still do occasional fingerprick checks and am confident in its accuracy.
At some level this data was “worse” than above. But maybe ok.
The TIR and TItR had both decreased a little. The CV had increased a bit (meaning more variation). The lab HbA1c had increased to 5.4% (even though this particular eHbA1c estimate was 5.1%).
None of those were terrible changes, but notably my TBR (<3.9) had increased to 4.2%. Even though most of that was just below 3.9, this had passed that 4% “minimum goal”. I wasn’t especially happy about that. Especially as the time below 3.6 mmol/L had increased too.
CGM coverage was still over 99%. However…
Confounding factors – CGM cost
This was in the time before we had CGM subsidised for T1 in Australia. So I had a financial incentive to stretch out my CGM sensors as much as possible. I would sometimes run the G6 sensors out to 16-20 days (this was less than I used to get with G5). But it was usually only when I saw the first signs of sensor failure or “noisiness” that I decided to start the replacement up (hoping the old sensor would last until the new one had stabilised).
Although I had been using overlapping sensors/transmitters for a while, G6 sensors take a lot longer to stabilise after insertion than G5 sensors did (especially as I didn’t use G5 in “native” mode). Mind you after that they’re a lot better, but it left me exposed to the wonky “tail-end” behaviour of sensors.
So a bit of that 99% of CGM data included false “compression low” data from the ageing sensors. Maybe my TBR wasn’t quite as bad as it looked, but I still wasn’t comfortable with it. This may have also had some correlation with the 0.3 difference between eHbA1c and HbA1c, although it’s not uncommon for me to see variations of 0.2.
AGP
The clinical statistics may have “degraded” a bit, but my endo agreed with me that the change in lifestyle was worth a lot too. And basically in her eyes the clinical results were “more than good enough”. In fact she still sometimes uses the word “ridiculous” when describing my results.
What it was like
I’ve written before about the huge psychological difference in life when you can mostly leave the system to look after things by itself to deal with the minutiae.
I do remain conscious of what I’m eating (having coeliac disease means I always need to be careful) and how much. But that’s in much looser terms than in counting carbs/protein/etc. I get up in the morning, marvel at the CGM data on my watch, have breakfast, get on with my day, and eat and drink as I feel like it. Occasionally my watch might alert me that I’m dropping fast (typically there’s some unannounced incidental exercise that takes the blame) but a quick snack fixes it and I rarely have to stop what I’m doing.
However, I did feel it could be better clinically. Even fewer lows (and low alarms!) would be good. I’d had excellent stats before so while these weren’t “bad” statistics, I knew that better was possible.
This snapshot was actually a highlight. As you’ll see on a later graph, in this period I was usually managing ~85% TiTR and ~95% TIR. I was happy with that, but if I could improve the TBR and the CV I’d be happier. And of course, if the HbA1c came down a bit at the same time I wouldn’t be unhappy. After decades of being measured by HbA1c it still seems to have psychological impact.
Fully-Closed Loop, 2023 |
(to start) |
A year later, and I’m currently using Lyumjev insulin (which I’ve brought from overseas as it’s not yet approved in Australia).
I have continued to make changes to my management though. As far as the AID algorithm goes, I’m trialling a variation which uses a scaled ISF model (but is otherwise traditional oref).
I also did things like raise my target BG from 5.1 mmol/L to 5.4.
While there can be hesitation about that target rise due to a sense that it may result in a higher average BG (and thus HbA1c) it should also mean the target is just that bit further away from a “hypo” classification.
But as my lab HbA1c results had not been outside the reference range since 2017, I decided I could afford to play with it a bit.
At the same time, CGM had received government subsidy in July 2022. In the lead up to that I decided that given my previous experience that I would try to start a new sensor every 12 days. That way ideally I could switch to each new sensor before the old one started getting things like extra compression lows. I’m still getting more than the standard 10 days out of each, but everything has become more predictable. And with usually no outage (such as for warmups/instability) between sensors.
Then at the beginning of March 2023 I started gathering a new set of data. Just prior to that things were a bit disrupted (with air travel and jet lag) so I decided a reset was in order. Some of above changes were part of this.
This dataset will have grown to my standard 60 days when I next meet with my endo, but so far it’s at least up to 21 days. You’ll recall that 14 days is generally accepted as a minimum timeframe for analysis.
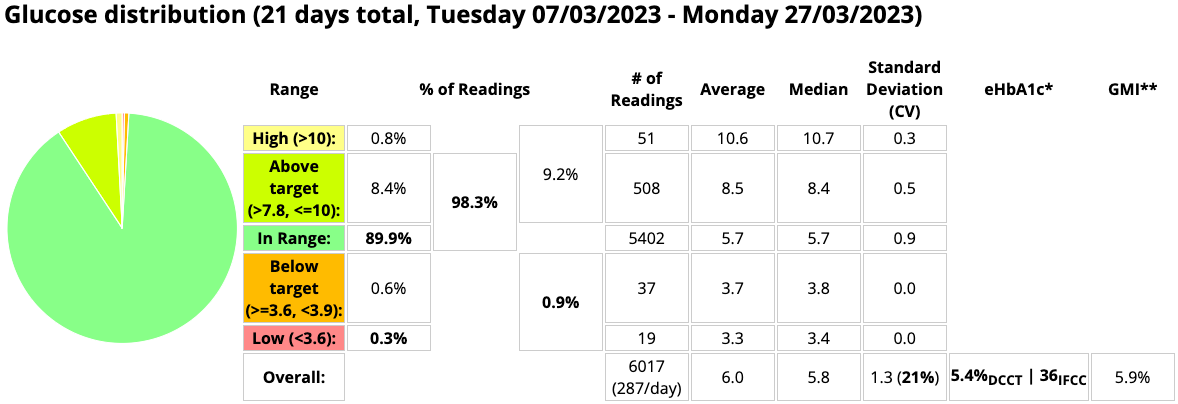
And a remarkable 21 days it has been!
What should be immediately obvious in comparison to a year ago is the reduction in both TBR and in CV, and the increase in TIR. Meanwhile the eHbA1c has hardly moved. A lab HbA1c test on the 27th gave 5.3% (although obviously that’s also being affected by data more than 3 weeks old). The CGM capture rate was 99.5% (I can almost hear that word “ridiculous” again).
That 0.9% of time below 3.9 mmol/L (70 mg/dL) averages out to fewer than two CGM samples per day. And fewer than one below 3.6 (65)!
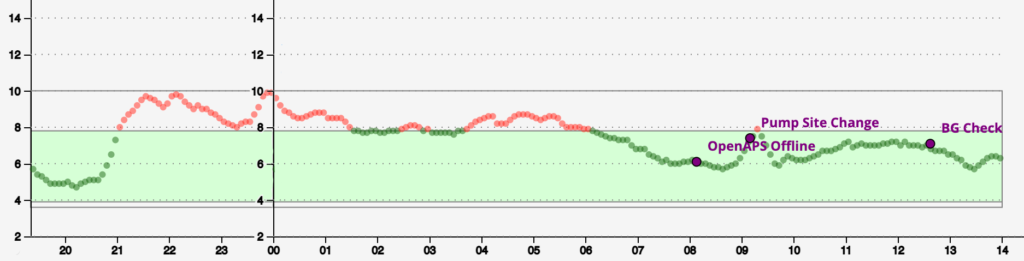
AGP
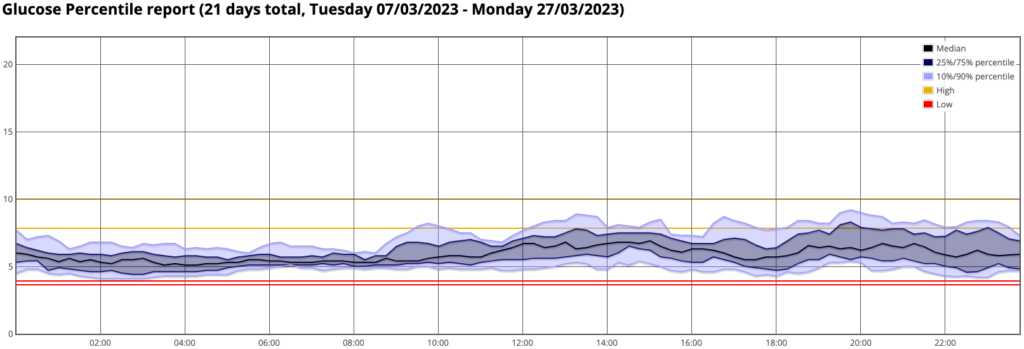
Here’s the percentile graph just for completeness.
It’s obviously a little “bumpier” than the previous graphs, simply because it contains a third the number of days.
Summary
Instead of comparing the latest results to a year ago, the comparison that leaps to my mind is to the last set of Hybrid Closed-Loop data in 2020 when I was doing a lot of manual interaction with the system.
| 2017 | 2020 | 2022 | 2023 | |
|---|---|---|---|---|
| Sample days | 60 | 60 | 60 | 21 |
| AID Mode | HCL | HCL | FCL | FCL |
| TIR (3.9-10) | 93.6% | 97.7% | 95.2% | 98.3% |
| TItR (3.9-7.8) | 70.8% | 93.6% | 89.2% | 89.9% |
| TBR (<3.9) | 1.3% | 2.0% | 4.2% | 0.9% |
| TBR (<3.6) | 0.6% | 0.5% | 1.7% | 0.3% |
| CV | 25% | 20% | 23% | 21% |
| eHbA1c | 6.0% | 5.1% | 5.1% | 5.4% |
| HbA1c | 5.8% | 5.0% | 5.4% | 5.3% |
| Comments | Started looping recently. | Excellent results. A lot of manual interaction. |
“Fully-closed”. Very little interaction. Wish fewer lows. |
“Fully-closed”. Seem to have cleaned many things up! |
For now the 2020 TItR shows a higher number, but still the current 90% does not make me sad! We’ll see how the 2023 numbers develop. But in the meantime I find the 2023 Time Below Range numbers to be remarkable!
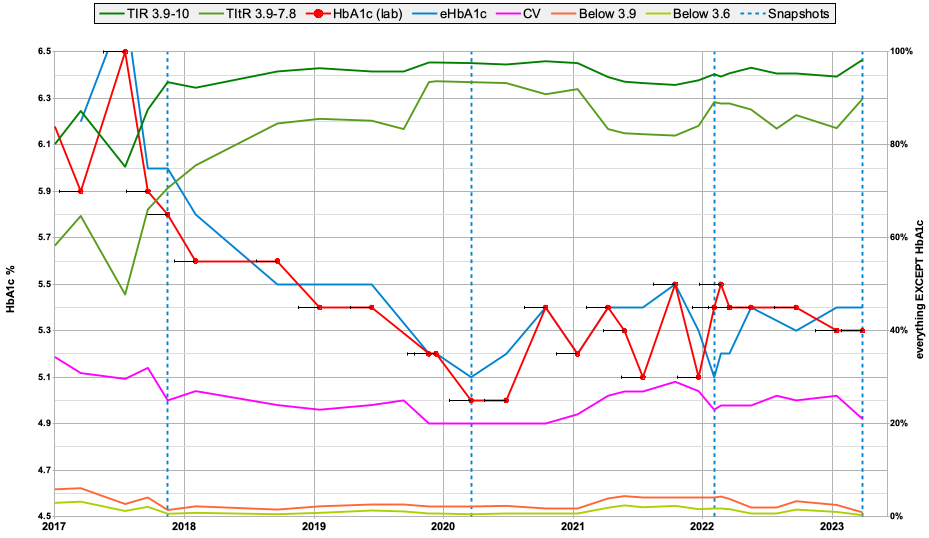
Now as you might expect, life hasn’t been as simple as just these 4 points in time. There’s been a bit of variation in between. But I’ve chosen those points to illustrate what feel are milestones I’ve been past.
Incidentally, that sudden rise in the TItR line in late 2019 correlates closely with my switch from Humalog to Fiasp insulin.
The HbA1c results have bounced around a bit in 2021-2022 (which seems to be the nature of that test) but it has generally been within 0.2 of the eHbA1c.
But it’s only 21 days of data!
Admittedly the right edge of that graph is based on 21 days, whereas the other points are based on 60 days. So maybe I’m just seeing normal variation and it might “average out” next week?
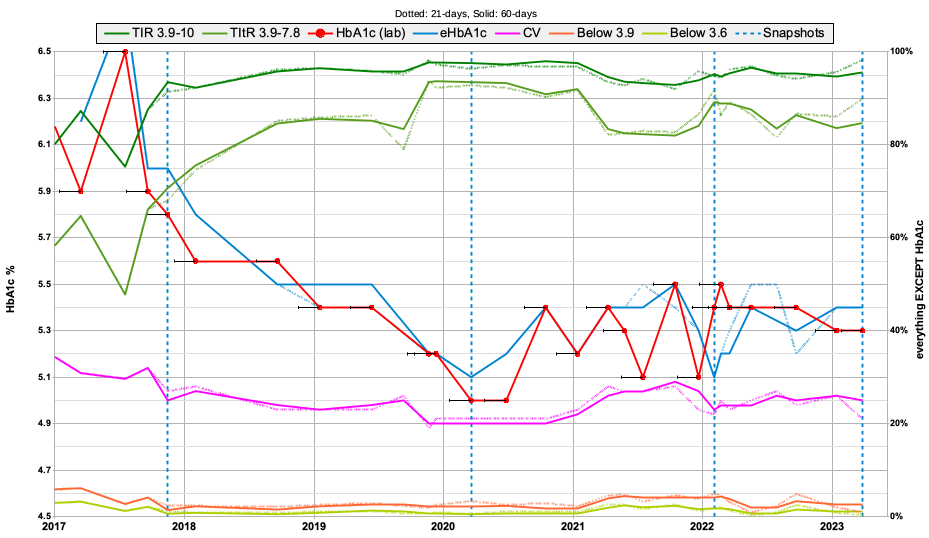
So here’s that same graph with the history re-analysed with 21-day data where available (the dotted lines).
Tap on the image and zoom in if you want a closer look. It gets a bit busy (especially around the HbA1c lines).
While there is usually some variation between the 21-day and 60-day data, I do think the difference on the very right of this graph is a lot more significant than most of the other examples. I do know I changed several things in early March after my return from Germany, which correlates with that. Yes I am hoping that the change remains consistent for at least another 39 days!
Around May 2022 the 21-day TBR (sub-3.9) stats did also get down to 0.9%. But the current situation seems different, as this time it coincides with both the TIR going up and the CV coming down significantly.
Why bother with so much detail?
At almost any point along this path I could have said that the results I was getting were “good enough”. They usually surpassed the goals set out in clinical guidelines. And to a large extent I have: I’ve been quite happy with the results throughout. But in the background I’ve still been working to improve things.
Part of why I’ve kept on tweaking has been to improve my health as much as I can. I’ve known those guidelines are just “outer markers” for the territory I would like to be in. Along the way I’ve been diagnosed with non-diabetes health conditions that have reminded me that I want to keep myself as healthy as possible (my cardiac issues at the end of 2019 are one example).
But clinical data is not the whole story. The work and lifestyle needed to keep up the clinical performance is an important factor. If I have to do too much work I’m at risk of burnout, and that’s a problem for many of us with diabetes.
Where I’ve been able to reduce the amount of work I have to do, then I think my quality of life has improved. And that of my immediate family. Dinner is so much easier for everyone when we’re not bothering to track the weight of all the ingredients!
Is this low-carb?
Nope. Not by a long shot. I have written about that perennial question before (see “Yeah, but you’re low-carb“).
I am roughly conscious of how much I’m eating. I do try to avoid over-consumption. But I don’t count my carbs. Or my protein, or fat.
I eat meat, fish, veggies, desserts, etc. To keep everything safe and gluten-free we do home-cook a lot of meals, but we do occasionally get take-away or eat out too. I won’t hesitate to have some slices of regular GF toast with peanut butter if I’m hungry (and that stuff is not low-GI nor low-carb!). I generally drink water, sometimes some no/low-carb sparkling drinks, sometimes cider, sometimes gin. I rarely hesitate to eat chocolate (as long as it’s GF). Although if I’ve already eaten a whole 180g block of it today (or a pack of chocolate hot cross GF buns – Easter is approaching) I will probably resist eating another one too soon.
Unusual meals
I do not use my AID system as an excuse to be silly and over-consume. I do usually try to eat sensibly. Most of the time…
On a trip to Germany last month I was out with some #dedoc Voices friends and ended up in a restaurant that did not have a very gluten-free-looking menu. While others had various dishes (some crumbed, and many with an assortment of deep-fried components – thus at risk of gluten) I decided my safest option was a large bowl of nachos/cheese/etc. Probably intended for many people to share. I ate the whole thing, and it was quite nice.
Of course, that’s not the healthiest thing to be eating every day, but an occasional splurge shouldn’t hurt me. As it turned out, all the fat in the cheese combined with the carbs in the corn chips to give a long and extended carb impact. Although I didn’t go above 10 mmol/L, I did stay above 7.8 for much longer through the night than normal. But after a night of solid sleep I was back at around 6.0 mmol/L come morning. After breakfast and a scheduled (3-day) cannula change I was back for more conference sessions.
Life is meant to be lived
This is not about closely controlling and restricting my lifestyle:
- I don’t closely monitor my BG or give myself injected corrections to avoid highs or rescue carbs to avoid lows.
OK, I do occasionally have a snack if I notice I’m heading low, but that feels normal.
I do glance at my watch on occasion just to convince myself everything is still working, but I don’t think that counts as “closely monitoring”. - I don’t tightly restrict my diet (I do try to stay healthy though and not put on too much weight).
- I do try to get a reasonable amount of exercise (usually either using my bike or my feet to get places, or on mundane things like working in the garden).
I have seen the way some other people still have to put a lot of work into constantly managing their diabetes, and that just makes me feel tired!
I may have lived with Type 1 diabetes for over 40 years now, and it was 27 years before I got a pump and 34 before I got a CGM. But now it’s my AID system’s job to do all the hard work and take care of the minutiae. And I’m happy to say that it seems to be doing a very good job of it!
Now what?
It now seems as though I’m getting back to the sort of clinical data I was getting in 2020. But the major difference is I’m not having to work so hard. So where to now? As they say: “onwards and upwards”.
Well, hopefully I can keep it up of course. As mentioned I have several recent changes at play at the moment. I haven’t spelt out all the details here: hopefully over the next month or so I can identify the contribution of each without throwing the overall behaviour off. It would be nice if the data remained consistent when it’s out to 60 days and I’m next meeting with my endocrinologist.
As long as everything else stays stable, I suppose the obvious target will be to further improve the TItR number. But there is always the Law of Diminishing Returns to consider!
And there’s always room for further improvement in terms of usability, robustness, changing technology, etc. And work continues in order to make these tools available to as many people as possible. As part of that, my experiences should be useful for participants in the Close-It clinical trial I’m involved in.






Amazing results…seems better than “healthy” people would achieve..?
Amazing are your small variations…i don’t achieve this even without eating or moving ???